Rheumatoid Arthritis and Podiatry
Posted on 9th August 2020 at 12:10
Rheumatoid Arthritis RhA is an autoimmune condition that causes the immune system to attack the joints in the body.
Up to 90% of people living with RhA will develop symptoms in their feet.
These symptoms can present as pain or stiffness in the feet, warmth and swelling in the joint of the feet and aching after activity or standing for long periods.
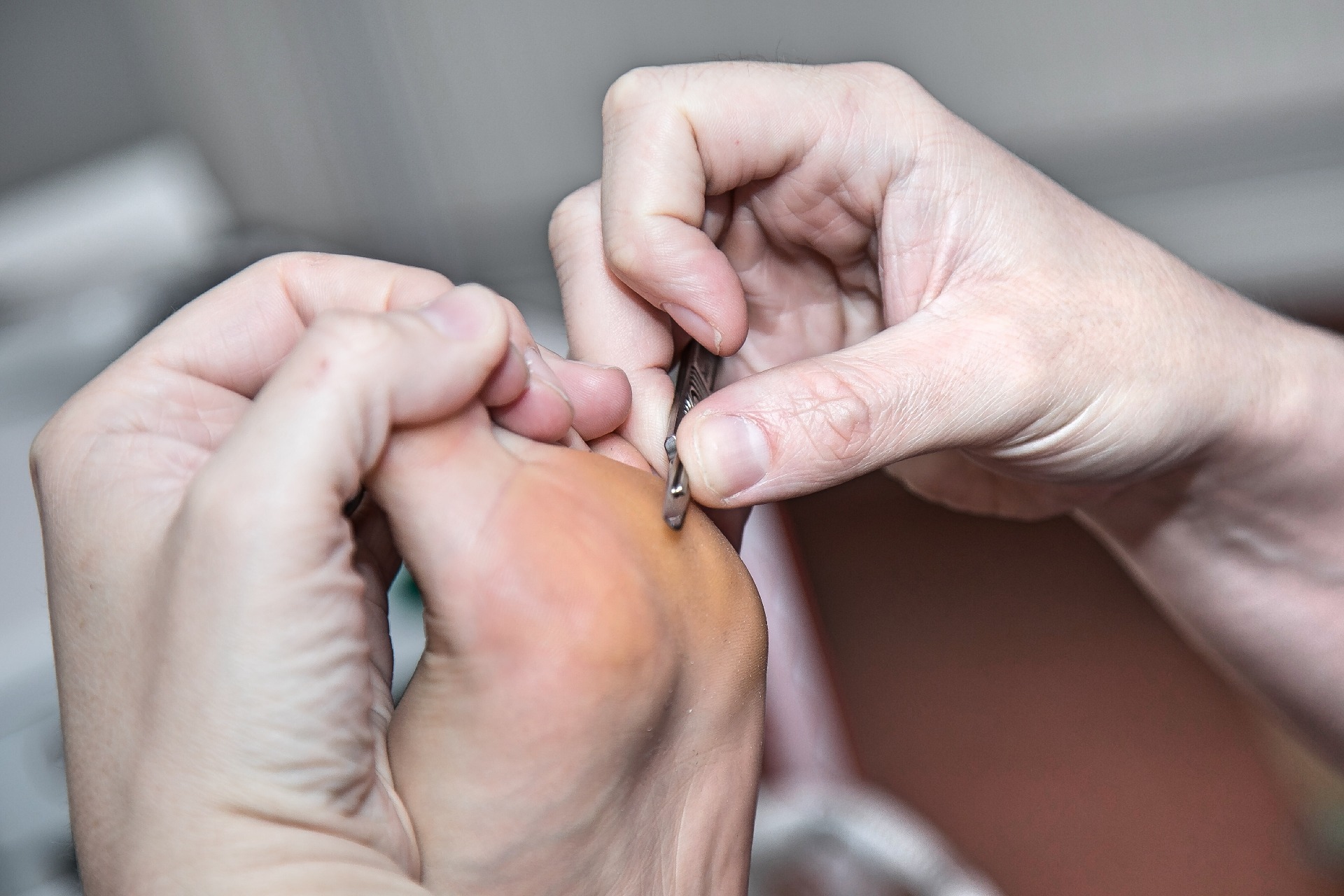
There are 33 joints in each foot so you can see why the feet can be become such a problem for people living with RhA as each joint can be affected, and, well we kinda need our feet to be pain free so we can walk comfortably.
Unlike Osteoarthritis where movement can help relieve symptoms when you are having a RhA flareup off-loading the foot is best. Podiatrists can help manage these symptoms and prevent the deterioration of the foot into the classic Rheumatoid Foot as seen here.
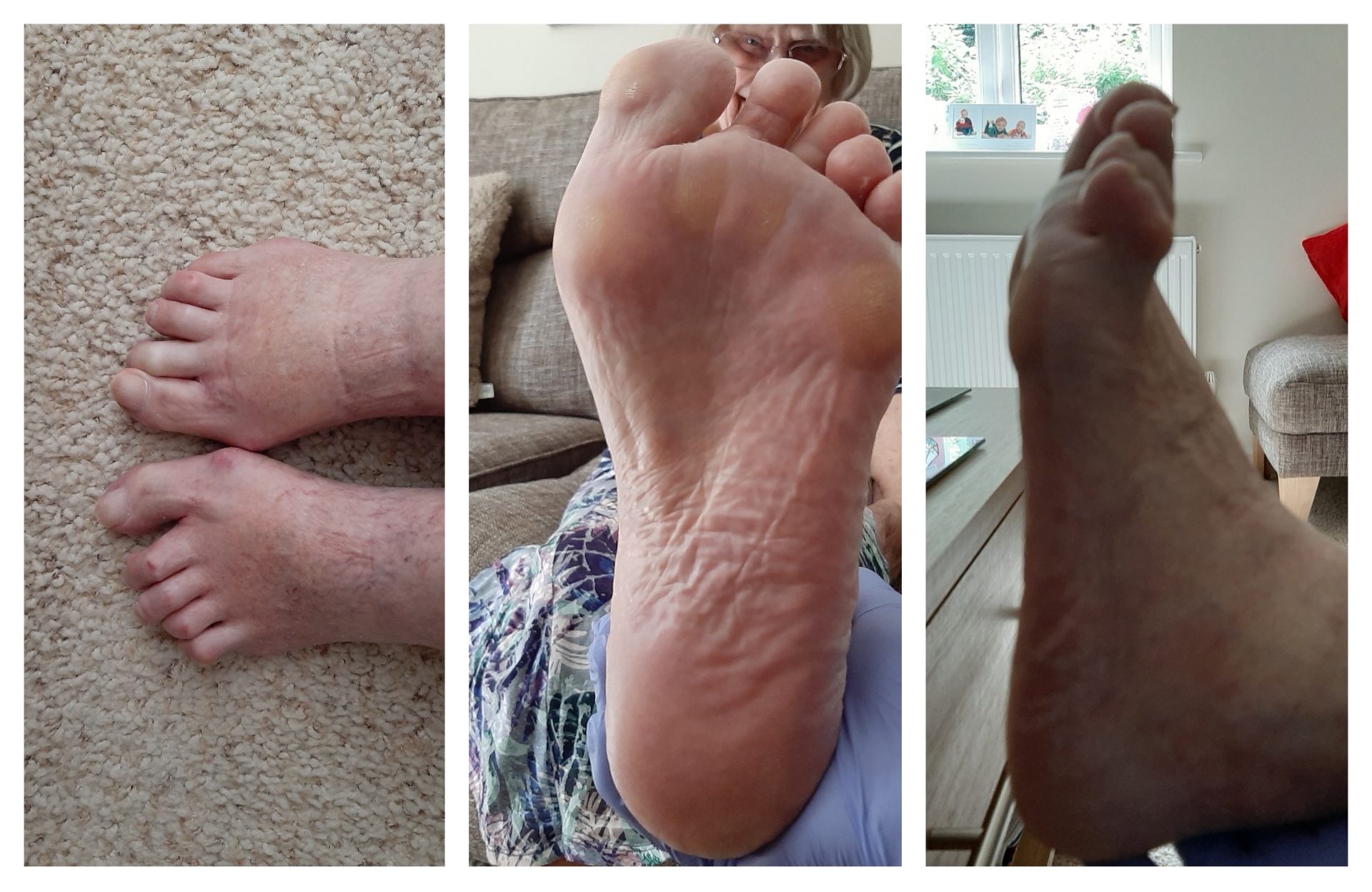
You may have heard of the ‘Classic Rheumatoid Foot’ (You must have, I mentioned it earlier). This develops due to joint destruction as the bone and cartilage break down.
Typically, this involves, retracting, clawing, or hammering of the smaller toes and bunions or trigger toes affecting the big toe area. The toes pulling back is usually combined with a tight, high arch and prominent bones in the ball of the foot. Callus can occur over the knuckles of the toes and the bony prominences in the ball of the foot. The fatty pad that normally protects the sole of the foot deteriorates and gets pushes away from the areas which need it most and this can cause pain, increased pressure and a feeling described as like walking on marbles. This foot type is weaker and has poor shock absorption due to its rigidity.
Other complications of the foot in RhA include:
BURSAE – these are fluid filled sacs caused by friction that often occur between joints or under the ball of the foot. They can be painless but if they become inflamed, now called a Bursitis, they can be painful.
Nodules – these are firm lumps in the soft tissue that can look white when you apply pressure e.g. standing. They are commonly found in the heel pad or over the Achilles tendon. Though not harmful or painful they can become rubbed by footwear and infected so definitely an area to be aware off.
Circulation – decreased blood supply to the lower limb associated with a hardening of the arteries can cause cramps in the leg when walking.
Raynaud’s phenomena – a painful condition that causes the toes to go white, then blue and red in response to temperature changes.
Vasculitis – this is thankfully rare and presents as a skin rash that can ulcerate. It is associated with long term disease and often exacerbated by smoking.
Peripheral Neuropathy – if the small blood vessels that feed the nerves in the feet become damaged this can cause a reduction in sensation or occasionally pain.
It is not advisable to treat corns and callus yourself as over the counter remedies and blades can inadvertently cause sores and cuts that can lead to infection and if you are living with RhA you will know that you are more prone to tissue breakdown.
Book regular trips to a podiatrist to reduce your callus and corns, a podiatrist will also assess your vascular and neurological supply and can spot problems before they occur. Podiatrists can provide immediate pain relief from bursitis using padding and strapping to offload the area and orthoses to prevent recurrence. Offloading the foot is a term used by podiatrists to describe the redistribution of pressure from a problem area into another part of the foot. This can help reduce hard skin, corns and ultimately ulcerations.
Customised orthoses can be prescribed to reduce areas of pressure, improve foot function, and prevent the deterioration of your feet.
Our aim is to keep you moving, keep your feet fit and healthy and prolong the integrity of your feet in spite of your Rheumatoid Arthritis.
Tagged as: Rheumatoid Arthritis
Share this post:





